Gardasil, a vaccine against human papilloma virus (HPV), which causes cervical cancer and genital warts — is now available across the United States.
Before we start discussing the vaccine, let’s have a clear understanding of what it tries to avert.
What is HPV?
According to WebMD, “HPV is a group of more than 150 related viruses. Each HPV virus in this large group is given a number which is called its HPV type. HPV is named for the warts (papillomas) some HPV types can cause. Some other HPV types can lead to cancer. Men and women can get cancer in the mouth or throat and anus or rectum caused by HPV infections. Men can also get penile HPV cancer. In women, HPV infection can also cause cervical, vaginal, and vulvar HPV cancers.”
Sexual activity is what spreads the virus. It’s one of the most common sexually transmitted diseases (STDs) in the country, according to the Centers for Disease Control and Prevention (CDC), with more than 20 million people currently infected and another 6.2 million getting the virus each year.
 Who developed a vaccine?
Who developed a vaccine?
With the alarming rise of HPV cases around the world, the search for a preventive method was at full speed. Ian Frazer and his colleagues were the first to develop and patent the basic technology behind the HPV vaccine at The University of Queensland, now marketed as Gardasil. Extensive studies proved that vaccinating young women with a Gardasil significantly reduced cervical cancer diagnoses and deaths, as well as a significant number of cervical screening abnormalities. The HPV vaccine also protects young girls and adult women from cancers of the vagina, vulva, and anus.
What is Gardasil?
Gardasil is a vaccine that protects against four HPV types (6, 11, 16, and 18). It is approved by the Food and Drug Administration (FDA) for use by females aged 9-26 to help prevent cancers of the cervix, vagina, and vulva; genital warts, and anal cancer. The vaccine also received approval for the use of males aged 9-26 to help prevent genital warts and anal cancer.
The Gardasil vaccine is made from tiny proteins that resemble the outside of the real human papillomavirus. It consists of aluminium, sodium chloride (salt), water, L-histidine, Polysorbate 80, and borax — A combination that stimulates the immune system and keeps the vaccine stable and suitable for injection. Gardasil does not contain any living virus, killed virus, or DNA from the virus, meaning it cannot cause HPV-related illnesses or any type of cancer.
Once the vaccine is administered, the body creates antibodies in response to the excess protein. The antibodies clear excessive proteins from the body, meaning if a person is then exposed to the real virus, the same antibodies can stop it from entering the cells and create an infection.
How is the vaccine given?
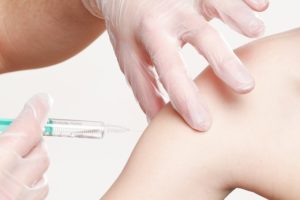
According to the Cancer Council, “Gardasil must be given as three injections in the upper arm. The vaccine works best if you have it over a six-month period, with the second dose of the vaccine two months after the first, and the final dose four months after the second (at 0, 2 and 6 months).”
How effective is the vaccine?
The HPV vaccine provides an impressive 100% protection against HPV types 6, 11, 16 and 18, particularly if all three vials are administered at the correct intervals, and if it is given before you contract an infection with these types.
Can both men and women receive the HPV vaccine?
In women, an HPV infection can cause cells in the cervix to grow abnormally. These HPV-induced changes develop into cervical cancer in a small percentage of women. Over 13,000 women are diagnosed with cervical cancer each year and roughly 4,000 women die from the condition.
HPV vaccines are incredibly effective at preventing HPV-related infections. Getting the HPV vaccine greatly reduces a woman’s risk of cervical cancer, and it substantially blocks precancerous growths. Men, on the other hand, may prevent the development of anal cancer, genital warts, and the spread of HPV to sexual partners. Gardasil is approved for males ages 9 through 26.
It is also important to remember that like all vaccines, Gardasil is a preventive method. The vaccine does not treat or cure an HPV infection in men or women who have already contracted the disease.
When should one get vaccinated?
HPV vaccine is routinely recommended for girls between the ages of 11 and 12 years. Doctors may recommend administering it to girls as young as 9 years old. The HPV4 vaccine is the type given in three doses to boys aged between 9 to 26.
It is crucial to get HPV vaccinated before the first sexual contact because the significant factor that drives the vaccine’s efficacy is the absence of HPV exposure. The vaccine can prevent almost 100% of disease caused by the four types of HPV targeted by the vaccine, especially when given at a young age.
For adults, re-vaccination is recommended if the vaccination schedule was not completed.
Who should not get vaccinated?
Pregnant women or individuals who are moderately or severely ill are discouraged to get HPV vaccination. It is also advisable to consult your doctor if you have severe allergies, including an allergy to yeast or latex. Additionally, if you have had a life-threatening allergic reaction to any component found in the previous dose of the vaccine, it is highly recommended to stop further administration.
Are there side effects to the vaccine?
In both clinical trials and real-world use, the HPV vaccine appears to be very safe. From 2006 to 2014, roughly 25,000 out of the 40 million vaccinated citizens reported to the government about HPV vaccine side effects. The most common side effects are minor, including:
- About one in 10 people had a mild fever after the injection
- About one person in 30 experienced itching at the injection site
- About one in 60 people had a moderate fever
Symptoms are quickly relieved without treatment. Other mild to moderate side effects can also include arm pain where the vaccine was injected, nausea, fainting, and headache. Overall, 90% of these cases were classified as nonserious.
Consult your general practitioner if you have not been vaccinated for HIV or if you detect symptoms of HIV.
For cancer treatments, get in touch with New Hope Medical Center
At New Hope, we offer a cross between conventional and alternative cancer treatments, with emphasis on improving a patient’s quality of life and addressing the cause of the disease. Call us today at 480-757-6573 to learn more about our treatments.

